A rising COVID signal in July is a clue to how the virus is different than other diseases we think of as seasonal illnesses.

www.thestar.com
What a rising summer wave says about Canada’s long-term future with COVID
A rising COVID signal in July is a clue to how the virus is different than other diseases we think of as seasonal illnesses.
Updated 6 hrs ago
July 27, 2024
5 min read
Save
Summer. A time for the hot, humid weather that tends to suppress familiar respiratory illnesses, like the flu.
Andrew Francis Wallace/Toronto Star

By
Megan OgilvieHealth Reporter
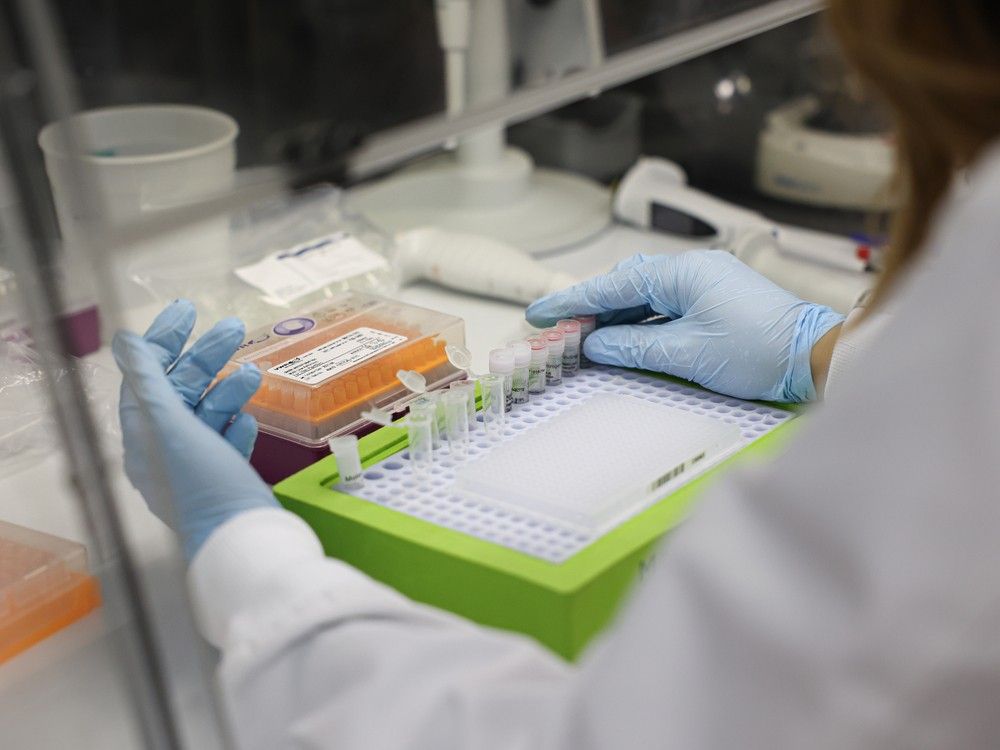
Your nose is stuffy. Your sinuses ache. Between a full-body sneeze and another series of phlegmy coughs, you start to wonder: Could this summertime bug be COVID?
The blazing hot days of July typically bring relief from a slew of respiratory illnesses. But across the country,
COVID-19 levels are swinging up, setting off a summer wave of sickness.
With many of us seeing the virus’s reach firsthand — even U.S. President Joe Biden
tested positive last week — it’s a clue to how COVID is different than other diseases we think of as seasonal illnesses.
In Ontario, the province’s wastewater signal is showing an uptick in COVID activity, with current levels similar to those reported in February during the winter respiratory virus season. As of July 25, the most recent data available from
Public Health Ontario, the GTA and eastern Ontario are seeing the highest COVID levels. National data also
reveals evidence of a fresh COVID wave.
“The trends have been going up over the last couple of months; we have about 50 per cent more cases circulating now than in May,” said Sarah Otto, a professor at the University of British Columbia and researcher with Canada’s Coronavirus Rapid Response Network, known as CoVaRR-Net.
“That’s unusual for a respiratory disease to go up and up and up during the summer months.”
Though this newest COVID wave is unlikely to surpass the
severity of a winter peak, experts say the current rise in infections is yet another signal that the virus is not going away.
“This virus continues to persist and be part of our environment,” said Dr. Andrew Pinto, a physician and public health specialist at Unity Health Toronto. “It’s shown that it can continue to surprise us.”
ARTICLE CONTINUES BELOW
What’s driving the summer wave?
The arrival of new variants has kick-started this new COVID swell in Canada, said Otto, an evolutionary biologist and Canada Research Chair in Theoretical and Experimental Evolution.
While many different variants are circulating, the ones “really taking off and doing very well” are those in the KP family, especially KP.3, she said. These variants have evolved to have more immune evasive properties and are better able to spread.
At the same time as these more infectious variants are flourishing, people’s immunity to COVID, whether gained from prior infection or immunization, is waning.
“A lot of people got infected earlier in the year and very few people got vaccinated,” Otto said. “And all of that immunity is slowly eroding, making it easier for COVID to infect people.”
In Ontario, KP.3 makes up nearly two-thirds of COVID cases in the province, according to the most recent data from
Public Health Ontario.
ARTICLE CONTINUES BELOW
Otto, who notes the KP family is part of the Omicron lineage — which rapidly spread around the world starting in late 2021 — said the KP lineage has evolved by the addition of mutations that help it evade our immune responses.
“That’s what makes us more susceptible; these variants are masking from our immune system just a little bit better.”
Not like the flu
Most respiratory illnesses have a six-month season in Canada, spanning from early November to late April, though the exact timeline depends on the year. Influenza and RSV, for example, fade almost completely in the northern hemisphere during the summer.
COVID is an outlier, said Dawn Bowdish, an immunologist at McMaster University who holds a Canada Research Chair in Aging and Immunity.
“There’s no evidence that COVID is going to fall into a seasonal pattern,” she said.
ARTICLE CONTINUES BELOW
Rather, waves follow the arrival of new variants as they capitalize on and break through waning immunity, said Bowdish, who notes Canada’s COVID trends tend to lag those seen in the U.S. and the U.K.
“There’s an infection pattern of these consistent waves of increased hospitalizations and increased peaks of infections that occur every three to six months.”
And while many common respiratory viruses — including COVID — thrive in cold, dry weather, Bowdish said COVID infects just as well in hot, humid weather.
“COVID doesn’t need help to spread. It doesn’t need any help at all.”
What next for wastewater surveillance?
In Canada, the data sources COVID experts use to understand viral activity, assess risk and inform public health measures and messaging are slowly being cut back.
Last month, the Ontario government confirmed it was
ending the wastewater surveillance program used to assess COVID activity in the province. The program — the largest of its kind in Canada — will end July 31. The province has said federal wastewater testing will expand in its place, though experts say the move drastically
reduces the number of testing sites in the province.
Otto added that national COVID data is becoming harder to access. She points to the federal government’s decision in June to stop sharing case counts.
“The problem with that is we don’t know who is being tested — and reported — and how this varies across the country,” Otto said. “We’re not getting that overall picture anymore.”
Bowdish said without consistent and easy-to-access data, including Ontario’s wastewater signal, it will be difficult for the public to assess their personal risk of getting COVID in the community.
Currently, she said, the most reliable data is on hospitalizations, a “reactionary” signal.
“It means you are responding when people have already been hospitalized and have had their lives affected by a serious infection,” she said.
ARTICLE CONTINUES BELOW
Pinto, a University of Toronto professor and director of the Upstream Lab at St. Michael’s Hospital, which works to address issues related to the social determinants of health, agrees that it is short-sighted to pull back on monitoring and other data systems that detect public health threats — for new COVID variants and for emerging viruses, such as highly pathogenic avian influenza.
At the Upstream Lab, researchers have an
ongoing study to test treatments for COVID, said Pinto, adding they’ve also launched an
initiative with primary care and emergency departments to help prepare for future pandemics.
“We don’t want to lose these things that we learned in the pandemic.”
‘Now part of our world’
Keeping up to date with vaccines and staying home when sick remain important protections during this fifth COVID summer, said Bowdish, stressing that immunization is especially critical for older adults and other vulnerable populations.
“We know that hospitalization with any serious respiratory infection, including COVID, can leave older adults with a litany of health issues, some of which they might never recover from. Preventing hospitalization is important.”
For the fall, the
National Advisory Committee on Immunization (NACI), is recommending those at highest risk get the most recently updated version of the COVID shot. Ontario has not yet released its plans for a fall immunization campaign.
ARTICLE CONTINUES BELOW
Despite clear evidence that COVID vaccines are safe and effective and have few side effects, immunization rates have dropped off in Canada. As of June 30, just
18 per cent of the population had received a vaccine targeting the XBB variant, which was rolled out last fall.
“(These vaccines) are protecting us from major disease; there’s still a lot of deaths from COVID,” said Otto, pointing to
data from Alberta that shows COVID continues to lead to far more deaths and more hospitalizations than influenza. “Yet, fewer people get the COVID vaccine compared to the flu vaccine.”
With Canada’s summer COVID wave rising, Pinto said people should have “a higher index of suspicion” that cold and flu-like symptoms are COVID, and recommends people continue to test and stay home when sick. Older adults and those who are immunocompromised can ask their health-care provider about getting a vaccine if it’s been a long time since their last COVID shot, and the general public should be planning for a jab in the fall, he said.
While many people want COVID to be over, Pinto said the virus can’t be put in the rearview mirror.
“This is a novel virus that’s now part of our world.”


 15%)
15%) 5%)
5%) 17%)
17%) 18%)
18%) 19%)
19%) 27%)
27%) 57%)
57%) 16%)
16%) 60%)
60%)
 0.4%)
0.4%) 0.1%)
0.1%) 0.7%)
0.7%) 0.1%)
0.1%) 0.5%)
0.5%) 1.1%)
1.1%) 1.4%)
1.4%) 1.0%)
1.0%)