Yommie
SpeedLimited
- Oct 2, 2013
- 64,184
- 37,190
- Country of Origin

- Country of Residence

- Thread starter
- #1,126
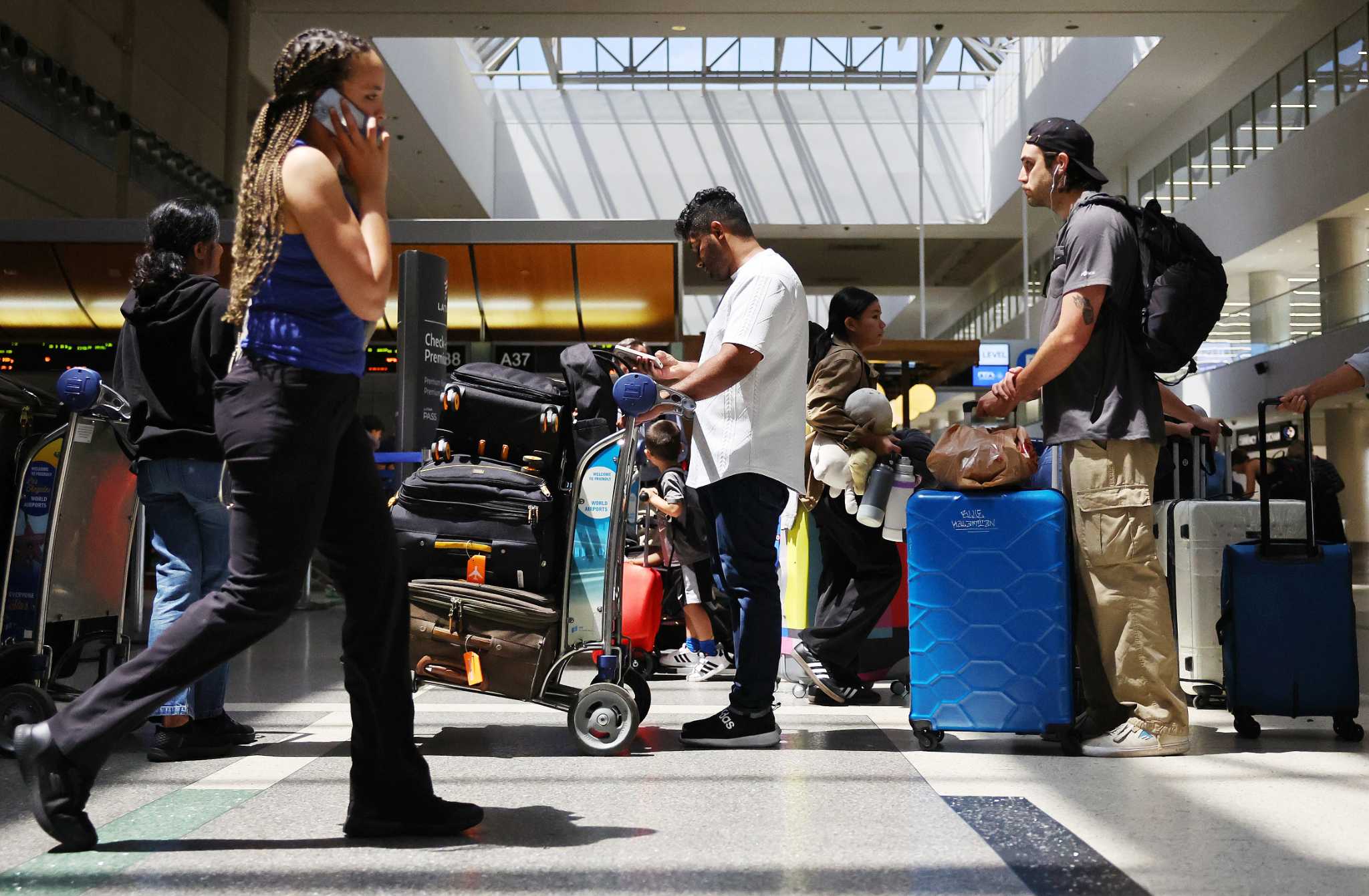
How California’s early summer COVID wave could affect travel and gatherings
Historically, California’s summer wave of coronavirus cases peaks around mid-July to late August. However, the virus remains unpredictable.
How California’s early summer COVID wave could affect travel and gatherings
By Aidin Vaziri, Staff WriterUpdated June 25, 2024 4:50 p.m.
California’s summer wave of COVID-19 cases, which usually peaks from mid-July to late August, has arrived early.
California’s COVID-19 summer wave has struck earlier than expected, threatening to disrupt travel plans, sleepaway camps and family gatherings.
Last week, emergency room visits in California rose by around 16% from the week before, with a test positivity rate increasing to 7.5%, the highest for this time of year since summer 2022.
According to the Centers for Disease Control and Prevention, California is among 39 states where coronavirus infections are rising, with no states or territories experiencing a decline for the first time in months.
While individual infections are no longer tracked, deaths, emergency visits and wastewater testing remain reliable indicators of community spread. COVID-19 accounted for nearly 1% of total deaths in California per the latest figures from the state Department of Public Health, up from 0.5% a month ago. Wastewater data from around the Bay Area show medium or high levels of SARS-CoV-2 at all monitored sites.
Historically, California’s summer wave of coronavirus cases peaks around mid-July to late August. However, the virus remains unpredictable.
An early COVID-19 summer wave in California threatens to disrupt travel plans, camps and family gatherings.
“For flu and for RSV, we have years and years of data with very similar trends over time. So, you can’t quite set your watch by when those seasons are going to start, but you can get close,” Ruth Link-Gelles, head of the CDC’s COVID-19 vaccine effectiveness research, said at a Food and Drug Administration meeting earlier this month. “For COVID, that’s not true at all.”
Nationally, the CDC’s COVID Data Tracker shows a test positivity of 6.6%, an increase of 1.2 percentage points from the previous week. Emergency department visits rose by 14.7%, hospitalizations 25% and death rates 16.7%.
The FLiRT variants KP.3, KP.2 and KP.1.1, which are named after the location of their spike protein mutations, continue to dominate and now account for more than 50% of U.S. infections, according to the latest CDC data. The new variant LB.1 accounts for another 17.5% and is rapidly growing.
Experts believe LB.1 may soon become the most prevalent strain, as it appears more infectious and better at evading vaccines or previous infections, according to a recent preprint study. The JN.1 strain drove a wave of cases last winter, and the rapid emergence of new variants has surprised some experts.
Last week, the FDA advised vaccine manufacturers to reformulate their fall shots to target the KP.2 lineage, reversing an earlier recommendation to target the JN.1 variant.
“These other new variants, these came up relatively quickly. I wouldn’t say they caught us by surprise, but because they happened relatively quickly, we had to react,” Dr. Peter Marks, an FDA director, said Friday at a webinar hosted by the group Champions for Vaccine Education, Equity and Progress.
He added that the switch wasn’t based on “iron-clad evidence,” but officials hope KP.2 offers marginally better protection.
“There’s probably some degree of cross-protection, but the optimal protection probably involves making sure we get closest to what is actually circulating now,” he said.
Here are some ways to prevent the latest COVID-19 wave from disrupting your summer plans:
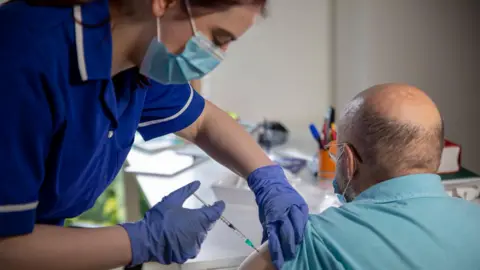
Infectious disease experts recommend wearing masks at airports, given the higher the risk of coronavirus transmission.
When should I wear a mask?
Consistent masking helps reduce transmission risk. It is especially advisable to use high-quality N95 or KN95 masks in situations such as public transportation, airports, airplanes, crowded indoor spaces and bustling restaurants. However, masks are generally unnecessary for outdoor activities, open-air events and alfresco dining.How can I navigate social situations and testing?
Use common courtesy and thoughtfulness when in social settings. Home test kits, though useful, have become less reliable for early detection. If symptomatic, consider multiple tests. PCR tests remain the gold standard but may be expensive. When visiting at-risk individuals, wear a mask and consider testing for the coronavirus beforehand to ensure their safety.What should I do if I am exposed or infected?
Follow CDC guidelines if exposed or infected. In case of exposure, wear a mask for 10 days, watch for symptoms and test yourself frequently. If infected, isolate if symptomatic and wear a mask around others. Those who have mild and improving symptoms, and are free of fever for 24 hours without the use of medication, can resume regular activities while wearing masks and avoiding crowded indoor spaces for at least five days.How should I prepare and pack for travel?
Pack high-quality masks such as N95 and KN95 models, coronavirus test kits, a thermometer and analgesics. Check that you have a plan for medical care at your destination and are up to date on your vaccinations to strengthen protection against the virus.What are the risks and safety strategies for air travel?
Wear a mask at airports and on planes, as the risk of transmission is higher in airports. Airplane ventilation is excellent once in flight. Older and immunocompromised travelers should be extra cautious and check that they are up to date on their vaccinations before traveling.As COVID-19 cases increase, public health experts recommend wearing a mask in crowded indoor areas and testing for the coronavirus before attending large gatherings.
Mauricio Santana/Getty Images